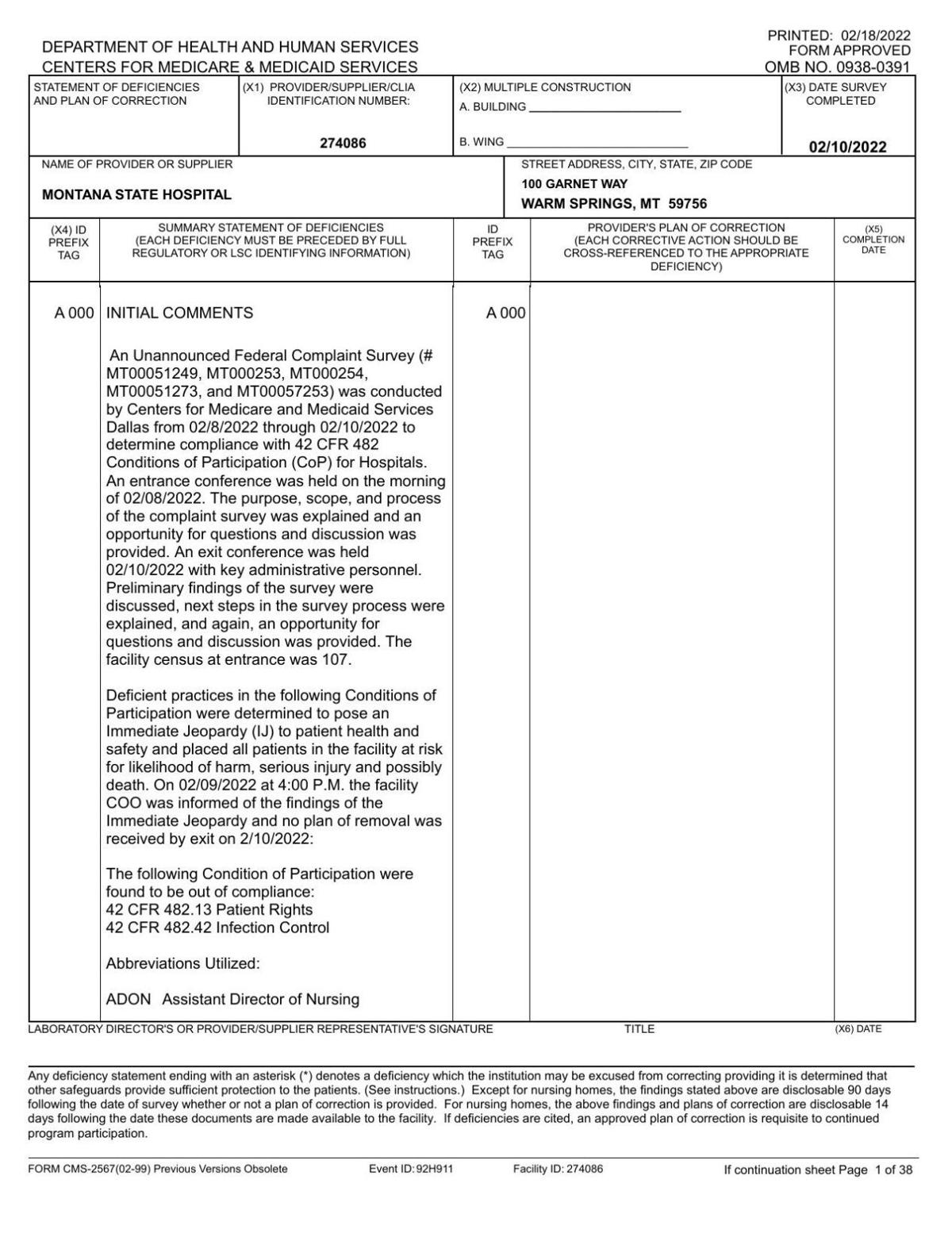
Kathy Toavs, a dementia patient at the Montana State Hospital, fell 13 times in less than two months before the last fall claimed her life.
The series of preventable incidents was noted by federal inspectors this month. The inspection, conducted by the Centers for Medicare and Medicaid Services, identified four patient deaths attributable to the hospital's noncompliance with federal rules.
The report following that inspection outlines the fatal consequences of failing to prevent patients from falling, as well as operating without a plan to contain a deadly COVID-19 outbreak inside the facility in Warm Springs.
According to that inspection report, obtained this week by the Montana State News Bureau, 87 out of 107 patients contracted COVID-19 in an outbreak the hospital failed to mitigate. Three patient deaths from COVID-19 could have been prevented had the hospital implemented precautions to reduce transmission of the virus, according to the report.
People are also reading…
Instead, some patients with and without COVID-19 were housed together, and when sick patients were isolated in certain units, staff were assigned to work COVID-positive and negative units, sometimes in the same day, according to the report.
Last week, the federal agency notified Montana State Hospital administrator Kyle Fouts that the facility has until March to correct the deficiencies uncovered in a three-day inspection earlier this month, or the facility would lose its federal funding.
In reviewing records documenting patient falls, inspectors found that Toavs died from pooling blood exerting pressure on her brain. Another incident resulted in a hospitalization.
Inspectors in February found hospital staff failed to implement safety measures to prevent patients from falling again and again.
Also, according to the report, staff did not complete assessments after some incidents and didn't keep one patient under 1-to-1 staff supervision despite repeated falls.
The inspection was a follow-up on another review of the facility in September, when CMS surveyors found patients had fallen 113 times between June and August 2021. According to the more recent report, 41 patients had fallen on four units between Jan. 1 and Feb. 9. The hospital census was 107 when inspectors arrived Feb. 8.
Ten of those falls were attributed to one patient, who died on Jan. 30 after one fall days earlier resulted in a subdural hematoma. The Montana State News Bureau cross-referenced the CMS report with death certificates of those who have recently died at the Montana State Hospital to identify this patient as Toavs. She was 74.

Kathy Toavs, 74, died Jan. 30 after falling from her wheelchair at the Montana State Hospital. A federal inspection found Toavs had fallen 13 times in less than two months, and that the state hospital failed to implement a plan to prevent her frequent falls.
"She loved her sons and her family," Roy Toavs, who had been married to Kathy for 53 years, said in a phone interview Tuesday. "We were pretty close to one another. If she didn't want to do something, I didn't either."
Toavs had suffered a stroke in January 2021, which started her on a winding path from hospital to hospital. That eventually ended with Toavs being admitted to Warm Springs on Aug. 8 with dementia, anxiety, diabetes and other diagnoses. Roy Toavs said his wife had a recent history of falling, so he wasn't surprised to learn from the report that his wife had fallen 13 times in less than two months leading up to her death.
According to the CMS report, hospital staff had assigned Toavs 1-to-1 staff supervision on Nov. 2, but the plan did not include interventions to prevent falls. The first recorded fall in the report identified an incident on Dec. 2, after which hospital staff assessed her to be a low fall risk. She fell again on Dec. 20 and 22. These incidents generated a higher fall risk assessment, although staff removed her from 1-to-1 supervision on Dec. 29.
Subsequent assessments varied from high to low over the next month, when she fell 10 more times.
It's unclear from the report why staff assigned her inconsistent risk assessments, despite a rapid increase in the number of times she fell.
Roy Toavs said his wife had told him during their occasional phone calls she wanted to be moved out of the state hospital and into a nursing facility. The report notes Toavs told the same thing to a behavioral health care planner on Jan. 18.
"I couldn't bring her home," Roy Toavs said. For 20 years he fetched what she needed when her diabetes made life challenging, but he's almost 74, has had several recent surgeries himself and said he would not have been able to hire someone in Wolf Point, their small Hi-Line community, to provide the care she needed.
On some days in January, Toavs had fallen twice in one day, sometimes an hour apart. In late January, she had reported falls four days in a row. Most incidents occurred without injury, although one fall noted she struck her head and staff observed a laceration on her elbow.
On Jan. 27, staff heard Toavs fall and found a bed sheet had wrapped around the wheel of her wheelchair. According to the report, blood was seeping from her left nostril and a physician noted swelling around her head and face. About two hours later, nurses were called to Toavs' room, where she was complaining of head pain and then "quickly became unresponsive."
According to the CMS report, hospital staff tried for about an hour to contact a house supervisor and two different doctors without success. When a nurse reached a third doctor, they called the Anaconda hospital and emergency medical services were sent to the state facility. Four days later, Toavs' son left a voicemail at the hospital notifying the staff Kathy Toavs had died on Jan. 30.
"The cumulative effects of these deficient practices placed patients at risk of serious illness and/or death," the CMS inspectors wrote in their report.
Roy Toavs said Tuesday he does not "want to be a negative person," and repeatedly said he understands the state hospital system is made up of people, and people make mistakes. He dearly misses his wife, less than a month after her death.
"I don't want to bash anybody and I know that this will probably not be the last case that happens this way," he said. "But hopefully (the report) can shed some light to help others a little bit farther down the line."
Outbreak control
The COVID-19 omicron variant that drove new case counts to unprecedented levels in Montana eventually made its way inside the Montana State Hospital, infecting 87 of 107 patients included in the survey from Jan. 4 through Feb. 8, as well as 95 employees across the entire campus.
Judy Knapp was another patient identified by the Montana State News Bureau through recent death records and the CMS report. She is one of three patients identified by CMS who died as a result of the hospital's failure to isolate and separate patients with COVID-19 from those without.
Knapp was an involuntary commitment to the state hospital, diagnosed with chronic obstructive pulmonary disease, diabetes and other illnesses, according to the report. She was admitted June 8, 2021.
Knapp's COVID-19 case predated the outbreak in January. She tested positive on Sept. 15, and experienced shortness of breath and fever through Oct. 3. She died on Oct. 4 from bilateral pneumonia, severe hypoxia, leukocytosis and COVID-19, according to her death certificate. She was 70.
Knapp had been housed on the Spratt Unit, the geriatric wing in Warm Springs that had tallied 28 COVID-19 positive patients through the January outbreak. Patients on that unit have high needs for cognitive treatment, and therefore could not be isolated on a unit designated to house COVID-positive patients during the outbreak, according to the report.
In a sense, it almost didn't matter: the B Unit, an admissions unit, had been set up to house COVID-positive patients, but only had space for eight patients and was quickly "overrun" with COVID-19 cases, the infection control officer told the federal inspectors.

The entrance to the campus of the Montana State Hospital at Warm Springs.
Inspectors pored through staffing documentation in the weeks before they arrived Feb. 8, and found some of the hospital units had been designated as COVID-19 units. But the growing number of infected patients and the crashing number of staff with COVID-19 soon overtook the facility's ability to maintain any separation, according to the report.
According to the report, one psychiatric technician's staffing paperwork showed they spent the first four hours of their shift on the B Unit, a designated COVID-19 unit, before being switched to E Unit, a non-COVID unit, for the next eight hours. Another psych tech on Feb. 6 worked on B Unit for four hours before moving to a different non-COVID unit for the remaining 12 hours of the shift.
On Feb. 9, the facility's infection prevention specialist told CMS inspectors, according to the report, "Currently the facility does not have an infection control plan, risk assessment or COVID-19 pandemic plan that has been approved … we only have rough drafts."
David Patzoldt, another patient whose death certificate matches specific information in the CMS report, had been admitted to the facility on Oct. 19 with major cognitive disorder. Patzoldt tested positive for COVID-19 on Jan. 14, and died Jan 26 from sepsis, COVID-19 pneumonia and cellulitis. He was less than two weeks away from his 76th birthday.
Inspectors interviewed the hospital's chief operating officer, identified in state employment records as Christopher St. Jean, who first said the hospital had dedicated staff for the COVID-designated units. Confronted with the staffing records, St. Jean said he was unaware staff was working both COVID-positive and non-COVID units, sometimes in the same day, according to the report.
The staff that tested positive include safety officers, direct care providers, business office employees, therapists, contract staff, dietary and administrative staff. According to the report, the quality assurance staff that received and interacted with the CMS inspectors at the beginning of the survey on Feb. 8 did not return the next day and later tested positive for COVID-19.
Fouts, the hospital's chief executive officer, was "out with COVID-19" when the CMS inspectors arrived, according to the report.
Inspectors note in the report they made the hospital aware on Feb. 9 that the hospital had reached "immediate jeopardy" status, which requires immediate corrective actions or the state hospital could lose its funding. The Montana Department of Public Health and Human Resources, which operates the state hospital, has said it is moving forward with corrective actions, but declined on Wednesday to describe its plan for corrective action.
DPHHS has declined to make Fouts available for an interview, but is working through the process of completing a $2.2 million contract for a temporary executive manager to oversee all of its health care facilities, with a focus on the state hospital. Lawmakers and employees in January opposed the decision to spend that money on a contracted management position, urging the department to instead turn those funds toward stabilizing the workforce.
Jon Ebelt, a spokesperson for DPHHS, said Wednesday the inspection findings do not change the scope of work for the contractor. The contract is expected to be awarded in March, Ebelt said.
Correction: An earlier version of this story misstated the date Montana State Hospital staff removed Kathy Toavs from 1-to-1 supervision. The hospital staff did so on Dec. 29.