- India
- International
Explained: Why kidney rackets thrive
The busting of yet another racket throws the spotlight on the shortage of kidneys to meet the demand. Donations from the dead are rare; experts say increasing these will reduce dependence on live donors.
 At least five such rackets have been unearthed in the last seven years, including one just last week in Pune, where documents were forged to show a donor was the wife of one of the recipients. (Source: Getty Images)
At least five such rackets have been unearthed in the last seven years, including one just last week in Pune, where documents were forged to show a donor was the wife of one of the recipients. (Source: Getty Images)The Delhi police recently busted a kidney transplantation racket that targeted poor, homeless people, with the surgeries being carried out at a two-storey house in Sonepat, allegedly by a class X dropout operation theatre technician. Several such others have been unearthed across the country over the years.
How common are kidney transplantation rackets, and how do they perform?
At least five such rackets have been unearthed in the last seven years, including one just last week in Pune, where documents were forged to show a donor was the wife of one of the recipients. In three of these cases, documents were forged to get the transplant done at a hospital authorised for such surgeries, unlike in the Delhi case where the surgery was done by unqualified personnel at an unregistered facility.
“Hospitals actually become the soft targets in such cases, when in reality the doctors or the committee members are neither trained nor empowered to identify and take action against forged documents. If someone says they are the wife of the recipient, how can a doctor say they are not? We need to punish those who are getting the documents forged and those who are forging them,” said Dr Harsh Jauhari, a renal transplant surgeon who has been an advisor to the Centre on transplantation.
In one case from 2018, a doctor and a nurse lured people to their wellness centre on the pretext of free check-ups. They then “diagnosed” many of the patients as requiring kidney transplantation. The doctor would cite a cost of around Rs 4–5 lakh, and the nurse would later contact the patient and say she could get it done in Haridwar for Rs 60,000. They would then remove the kidney while performing the so-called transplantation.
What does the law say?

Under the Transplantation of Human Organs and Tissues Act, 1994, amended in 2011 and 2014, organs can be harvested from deceased donors or from living relatives of the recipient (children, siblings, spouse, or grandparents, and grandchildren). The Act also allows unrelated donors such as relatives other than close ones, long-term friends, or in-laws, but prohibits any financial exchange.
All cases of living donations have to be scrutinised by an in-hospital committee to ensure no commercial dealing happens. In cases of unrelated donors or any case flagged by hospitals, an external panel examines all papers.
After the 2011 and 2014 amendments, the Act allows swap transplants and donations from cardiac dead patients (earlier, organs could be donated only by brain dead patients), and raised the punishment to imprisonment up to 10 years and a fine of Rs 1 crore.
Why do rackets target kidneys?
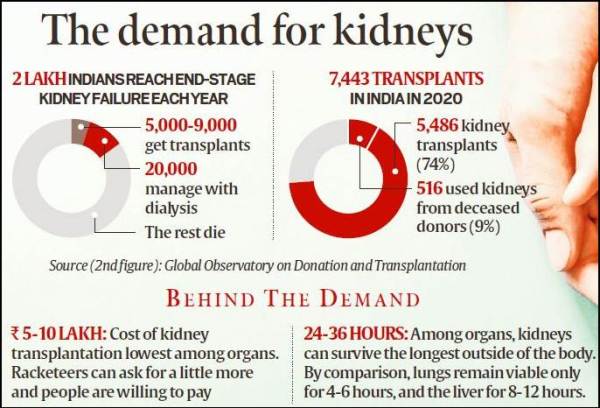
Although livers, pancreas, or lungs can be harvested from living donors, the rackets mainly target the kidney as it is the most in demand. Every year, an estimated 2 lakh people in India reach the end stage of kidney failure, requiring transplantation or dialysis, compared to 50,000 requiring a liver transplant. Only about 5,000 to 9,000 kidney transplant surgeries happen each year. “Another 20,000 are able to manage their disease with dialysis. The rest, unfortunately, die,” said Dr Jauhari.
The kidney can survive longer outside of the body — 24 to 36 hours — than the lungs (4-5 hour) and the liver (8-12). Transplantation cost is also the lowest for the kidney, at between Rs 5 lakh and Rs 10 lakh.
“These racketeers can ask for a little more and people are willing to pay because of the severe shortage. And, the quality of life after transplant is quite good. In fact, it is better than with dialysis, which is also costlier,” said Dr Vimal Bhandari, former director of National Organ and Tissue Transplant Organisation (NOTTO), the country’s apex network for coordination of organ procurement and allocation for organ transplant.
Newsletter | Click to get the day’s best explainers in your inbox
Again, India has expertise in kidney transplantation. “Most urologists these days are trained in performing a kidney transplant surgery. There are hundreds of centres across India that perform the procedure,” said Dr R P Mathur, senior consultant of nephrology at the Institute of Liver and Biliary Sciences.
Dr Jauhari added, “If you take for example liver transplant, it is a very big surgery and a lot of infrastructure is required. It also poses a higher risk to the donor. Kidney transplant has now been standardised and there is no undue risk to the donor. You can live happily with just one kidney.”
 Data from the Global Observatory on Donation and Transplantation
Data from the Global Observatory on Donation and Transplantation
What causes kidney failure?
The most common cause is hypertension and diabetes. Other causes include certain hereditary diseases, infections, and autoimmune diseases. “High blood pressure and diabetes are the biggest causes of kidney damage in India, leading to 50% of kidney failures. Obesity is also a big risk factor because it increases the risk of diabetes and hypertension,” said Dr Mathur.
He stressed the need for a healthier lifestyle for people to protect their kidneys. “Another problem is that people with diabetes and hypertension are not even aware that they have it, leading to more kidney diseases. It is important for anyone over 35 to undergo an annual health check-up. People with a family history of hypertension and diabetes must start at 30.”
What can be done to address the demand?
The only way to reduce dependence on organs from living donors is to increase donations from the dead, which account for a very small proportion of all transplants in India.
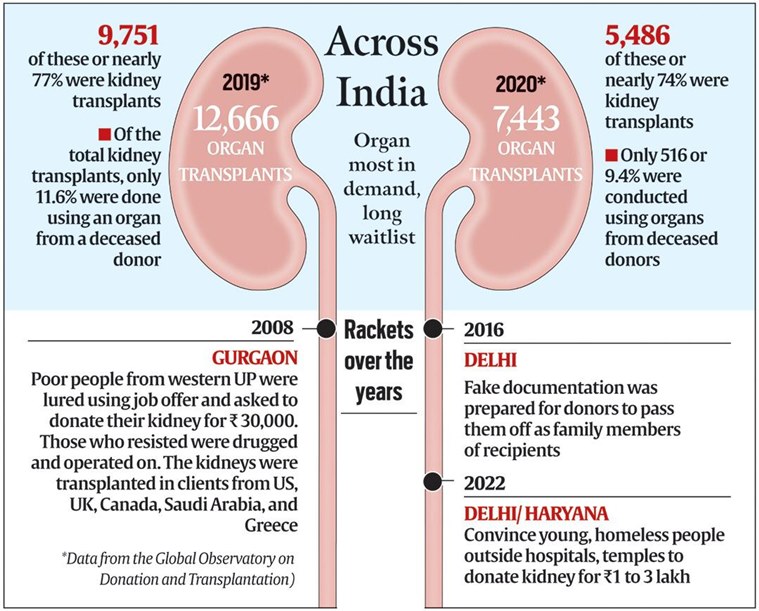
In 2020, there were 7,443 transplants in the country in 2020, of which 5,486 or nearly 74% were kidney transplants. Only 516 of the kidney transplants, or 9.4%, used organs from deceased donors, according to data from the Global Observatory on Donation and Transplantation.
“Over 1.5 lakh people die of trauma in this country every year. Even if we are able to motivate 70% of them to donate the organs, it will be of great help. But, deceased donations hardly happen in India because people believe various myths,” said Dr Bhandari. Trauma such as road accidents lead to the highest number of brain deaths, and these persons are ideal candidates for organ donation.
Experts said instances such as the unearthing of these rackets shake people’s faith, leading them to believe that harvested organs would be sold off by hospitals. People can start by pledging their organs to NOTTO. But it is essential that family members are on board. Even if a person has pledged her organs, these cannot be harvested if family members do not give consent after the person’s death.
More Explained
EXPRESS OPINION
May 08: Latest News
- 01
- 02
- 03
- 04
- 05












































